Enlarged Prostate – BPH
Benign Prostatic Hyperplasia (BPH) is a common, benign (not cancerous) condition in older men in which the prostate gland enlarges. The prostate is a walnut-sized gland that produces semen, the fluid that transports sperm. Located below the bladder and surrounding the urethra (the tube carrying urine out of the body), the growing prostate can squeeze the urethra and cause difficulty with urination.
Causes
Benign Prostatic Hyperplasia (BPH) is believed to be related to the aging process and the presence of the male hormone testosterone. More than half of men age 50 and older and 90 percent of men age 80 and older have BPH.
Symptoms
An enlarged prostate can cause a variety of urinary symptoms including: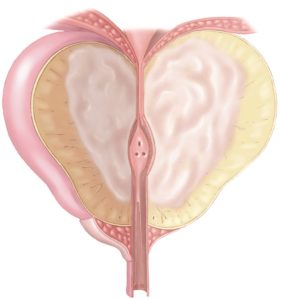
- Recurring, sudden need to urinate
- Increasingly frequent urination, especially at night
- Weak or interrupted urine stream
- Difficulty starting urination
- Urine leakage
- Inability to completely empty the bladder
- Blood in the urine (hematuria)
Caffeine, alcohol, spicy or acidic foods, certain cold medications, and constipation can make symptoms worse. Left untreated, symptoms may worsen over time and can cause complications that may include inability to urinate (urinary retention), bladder or kidney damage, bladder stones or urinary infections. See your doctor for a thorough evaluation.
Diagnosis
Our doctors and enlarged prostate specialists will take a medical history and do a physical exam. A digital rectal exam (DRE) will be performed. Your doctor may order a prostate specific antigen (PSA) test. Elevated levels of PSA can indicate BPH, prostatitis (prostate inflammation) or prostate cancer. Additional tests may include a symptom score sheet, a urine flow study, ultrasound, CT scan and a cystoscopy.
Treatment
Treatment for BPH / enlarged prostate will depend on the severity of your symptoms and how much they interfere with your lifestyle. Men with minimal symptoms may only need to make lifestyle changes; those with more pronounced symptoms or complications may require medication or a procedure. Your doctor can help you determine which treatment is most appropriate for you.
Lifestyle Changes
- Avoid caffeine, acidic drinks such as colas, tomato and orange juice, and alcohol. Cold medications containing antihistamines or pseudoephedrin, and constipation can make it more difficult to urinate.
- Limit evening beverages and urinate when you first feel the urge.
- Increase your physical activity level.
Medications
Recent studies indicate that using combinations of medications which work by different pathways may be more effective than a single medication to treat BPH.
Medications may include:
- Alpha blockers to relax the smooth muscle tissue in the bladder and prostate, increasing urinary flow
- Enzyme (5 alpha reductase) inhibitors to shrink the prostate by preventing the conversion of testosterone to dihydrotestosterone, a key ingredient in prostate enlargement
- Anti-cholinergics to reduce frequency and urgency
- Herbal products such as saw palmetto, derived from a plant in the Southeastern U.S., may reduce mild to moderate symptoms
Minimally Invasive Therapy
These procedures seek to open a passage through the prostate to allow urine to flow with less effort. Many are called “transurethral” because instruments are passed through the opening at the tip of the penis and into the urethra. Your urologist will perform the most advanced treatment using the least invasive technique appropriate to resolve your problem.
- Transurethral needle ablation (TUNA) – radiowaves heat and destroy obstructing prostate tissue
- Laser vaporization – a laser heats and vaporizes the obstructing prostate tissue
- Transurethral microwave therapy (TUMT) – microwave energy heats and destroys obstructing prostate tissue
- Transurethral incision of the prostate using electrocautery or laser
- Transurethral resection of the prostate (TURP) – obstructing tissue is removed through a cystoscope; more invasive than the preceding techniques, but urologists still use the results from the TURP as the standard by which other transurethral procedures are judged
- Prostatectomy – open procedure to remove the obstructing prostate; a less common option reserved for those with very large prostates
- Rezūm Water Vapor Therapy – a non-surgical treatment that uses water vapor to remove excess protate tissue with precision.
- UroLift – a minimally-invasive treatment using small implants the lift prostate tissue away from the urethra.
- GreenLight Laser Therapy – a laser is used to precisely and accurately remove overgrown prostate tissue.
- Aquablation Therapy – a minimally-invasive treatment using a high-powered waterjet combined with real-time imaging.
